Highlights
- Low energy availability (LEA) arises when there is not enough energy (calories) consumed to support critical body functions as well as extra physical activity, such as training
- Relative Energy Deficiency in Sport (REDs) is a result of longstanding LEA and is associated with a variety of negative health and performance outcomes
- Until recently, menstrual cycle patterns were considered a key indicator of energy availability in female athletes
- Menstrual cycles remain important, but ovulation is the key marker of energy availability
- This SIRCuit article summarizes the relationship between LEA, REDs and ovulation, as well as answers questions about whether ovulation monitoring is right for you
Am I eating enough to be healthy and perform at my best?
Researchers know now that assessing the adequacy of energy intake in athletes is not as straightforward as crunching the numbers for calories-in (the energy we consume through the food we eat) minus calories-out (the energy we use to function, from basic processes such as breathing and blood circulation to the complex processes we use to work or exercise). Be wary of what the latest calorie tracking app is promoting as one’s daily energy budget, as the cost of all the human body processes that are involved in energy consumption and expenditure is incredibly complex (Burke et coll., 2018).
What researchers, athletes, coaches and health practitioners are really after is an understanding of an athlete’s energy availability status. Energy availability (EA) refers to the amount of energy left over and available for your body’s functions after the energy expended for training is accounted for from the energy you consume from food (Loucks et coll., 2011). Inadequate energy availability, or low energy availability (LEA), arises when there simply is not enough energy (calories) consumed to support critical body functions as well as extra physical activity, such as training. If this goes on long enough, athletes can face serious health implications. Typically, physiological functions of the body get neglected and only receive the energy that is available after the needs of physical activity are taken care of. The prevalence of low energy availability is assumed to be high in female athletes, and if persistent may pose a significant health risk (Melin et coll., 2014).
 Relative Energy Deficiency in Sport (REDs) results from longstanding or severe LEA in athletes (Mountjoy et coll., 2014). It looks different in every athlete, and is associated with a variety of negative health and performance outcomes. For example, REDs can compromise physical (such as, reproductive, gastrointestinal, bone, and heart function) and mental health. It can also lead to impaired training adaptation, such as a decrease in muscle strength or endurance performance (Vanheest et coll., 2014; Woods et coll., 2017; Tornburg et coll., 2017; Schaal et coll., 2021) (See Table 1 for a list of Health and Performance Indicators of REDs).
Relative Energy Deficiency in Sport (REDs) results from longstanding or severe LEA in athletes (Mountjoy et coll., 2014). It looks different in every athlete, and is associated with a variety of negative health and performance outcomes. For example, REDs can compromise physical (such as, reproductive, gastrointestinal, bone, and heart function) and mental health. It can also lead to impaired training adaptation, such as a decrease in muscle strength or endurance performance (Vanheest et coll., 2014; Woods et coll., 2017; Tornburg et coll., 2017; Schaal et coll., 2021) (See Table 1 for a list of Health and Performance Indicators of REDs).
Why does this matter to athletes? Like a house with a poor foundation, the body eventually starts to “break down.” Without a solid health foundation, the athlete is susceptible to an increased risk of injury, illness and blunted responses to training, all of which may hinder sport performance (Mountjoy et coll., 2014; Vanheest et coll., 2014; Woods et coll., 2017; Tornburg et coll., 2017; Schaal et coll., 2021; De Souza et coll., 2021; Joy et coll., 2014; Heikura et coll., 2021, 2018).
So back to the question, how do we know a female athlete’s energy availability is in a good place? Until recently, menstrual cycle patterns were touted as one of the main indicators of energy availability status in female athletes. Once an athlete’s period arrived each month, the athlete and their respective support teams would be content, and training would go on. So, what has changed?
Menstrual cycle patterns remain an important element in understanding energy availability status, with missed menstrual cycles ringing the alarm for REDs risk. However, ovulation is the more important part of the picture when it comes to providing a lens to energy availability status. Confirming ovulation via the luteinizing hormone surge is now considered the gold standard to monitor REDs in female athletes (Elliot-Sale et coll., 2020, 2021).
Accordingly, if you are a female athlete who is keen to understand your REDs risk, or are a coach or parent of a female athlete, read on for an explanation of this method and walk away with a greater understanding of ovulation monitoring to support long-term health and performance.
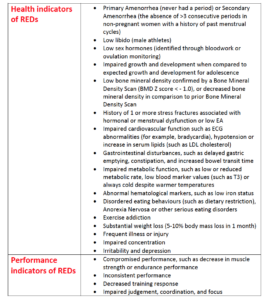
Table 1: Potential indicators of REDs (Mountjoy et al 2014; Woods et al 2017)
Common questions regarding ovulation monitoring
Is ovulation monitoring appropriate for me?
Before adding ovulation sticks to your shopping cart, it is important to understand if monitoring is a fit for you. If you experience a consistent period, every 21 to 35 days, or experience irregularly long or short periods, (more than 35 or less than 21 days), go ahead and purchase those sticks, ovulation monitoring is likely valuable for you.
However, if you are an athlete that is pregnant, breastfeeding, or menopausal, ovulation monitoring might not be appropriate for you due to hormonal influences at play. Ovulation monitoring is not a fit for those who have been exposed to hormonal therapy or certain medications or diseases that cause disruptions to the menstrual cycle over the last six months. This includes oral contraceptives (“the pill”), hormonal IUDs (such as Mirena), estrogen, progesterone, and testosterone. If in doubt, ask your doctor if ovulation monitoring is appropriate.
My period is like clockwork, but I’m still experiencing signs or symptoms of REDs. Do I really need to monitor ovulation?
It is highly recommended you monitor ovulation if you are experiencing symptoms of REDs (See Table 1). Regular menstrual bleeding does not always indicate ovulation and normal menstrual function. In fact, one study of recreationally active women (running around 30km per week) observed that 12% to 20% of the participants demonstrated anovulation (lack of ovulation) despite reporting regular menstruation (De Souza et coll., 1998; Prior et coll., 1990). This emphasizes the importance of monitoring ovulation and not just menstruation (in the form of bleeding), as ovulation is the primary indication of normal hormonal function. It is also important to be aware of other indicators of REDs beyond reproductive function (See Table 1).
 So I pee on a stick, is that right?
So I pee on a stick, is that right?
Ovulation sticks (not to be mistaken for pregnancy tests) can be purchased online or at a pharmacy. Approximately 20 to 40 sticks are needed to monitor for the recommended monitoring window of 3 months. Ovulation testing begins 7 days after day 1 of a new menstrual cycle. For those not currently menstruating, monitoring begins right away. Though different brands can promote different protocols, we recommend to measure every morning, first thing. This is because the hormone we are measuring, luteinizing hormone, generally peaks during the 12:00 pm to 8:00 am window (World Health Organization 1980, Cahill et coll.,1998).
Do you prefer a visual of the ovulation monitoring method? If you’d like to see a visual of the ovulation monitoring method, check out this infographic.
Every morning? How am I supposed to remember that?
We know. We get it. You’re busy. As a cue to remember, place the sticks on your bathroom sink, or the top of the toilet lid, as a visual reminder.
What happens once I get a positive test (or don’t)?
A positive test represents the luteinizing hormone surge that confirms ovulation (a good thing, in this case). Once you get a positive test, you can stop monitoring. Repeat the protocol outlined above for the next 2 cycles, with one exception: monitoring begins 7 days before the day a positive ovulation test occurred during the first cycle. For example, say, you ovulated on Day 12, you would start monitoring on Day 5 (7 days before) this time around.
If no ovulation occurs, test daily until your next menstrual cycle. Then stop monitoring until the cycle is complete and begin monitoring again the day after your cycle is over.
Initial ovulation monitoring should be conducted for a minimum of 3 months, and then repeated throughout the year depending on ovulation test results and recommendations from your physician.
What do I need to do with all this information?
Documenting the date and times of menstrual cycles and ovulation during this monitoring window is important to understand menstrual trends. It is also useful information to share with your doctor so all facets of your health are considered and assessed appropriately. Whether it be a calendar and pen, or tracking in your phone, determine what tool works for you and get tracking.
What if I haven’t gotten my period in a long time or I’ve never had a positive ovulation test?
If you are an athlete that has not gotten your period or a positive ovulation test, don’t ignore these warning signals. See your doctor right away, as missing periods or ovulations could be the body’s way of telling you that something is not right, including LEA or REDs.
If I ovulate and menstruate consistently, am I in the clear of LEA and REDs?
Menstruating with positive ovulation results is a very encouraging sign you are in the clear of LEA and REDs, especially if you don’t demonstrate any of the other signs and symptoms of REDs. However, if you still suffer from some of the symptoms of REDs, despite menstruating and ovulating, you might need to seek an assessment from a sports medicine physician. REDs could still be a factor, but showing up in your body in other ways (See Table 1 for Health and Performance Indicators of REDs).
Although monitoring might seem like a lot of work on top of training, the reward versus perceived inconvenience is huge. If you are a female athlete, consider adding ovulation tracking as part of your monitoring routine, as it could be very valuable to understand how you are faring physiologically and your risk for LEA and REDs. After all, a huge part of being a successful athlete and a healthy human involves tuning-in and connecting to one’s body cues to support long-term health and athletic success.
For more information, including an extended protocol and infographic on ovulation monitoring, visit the Canadian Sport Institute Pacific Nutrition Resources webpage.
 So I pee on a stick, is that right?
So I pee on a stick, is that right?